Ear Infections in Adults and Children
What is an ear infection? An ear infection is a condition that can cause pain in the ear, fever, and trouble hearing. Ear infections are common in children, but they can occur at any age. Middle ear infections (otitis media, OM) are among the most common reasons for visits to health care providers, and for prescribing antibiotics. Ear infections become less common after 3 years of age and are uncommon in adolescents and adults. People at higher risk for infection include those with family history of OM, bottle fed (not breast fed) infants, smokers and children of smokers, children in daycare, people with impaired immune systems, and people with prior history of OM. The occurrence of OM also increases during allergy season when pollen and other allergens are increased in the environment. Children who have not suffered an ear infection before age three are very unlikely to get them at an older age.
Vaccinations such as pneumonia and H. Flu (Hib) have been found to reduce the occurrence of OM, in addition to preventing the primary infections caused by these bacteria. For this reason, among others, the occurrence of OM has decreased in the United States in recent years.
What causes ear infections?
The typical course of events is:
● A triggering event such as a viral upper respiratory infection (URI or cold) during a time when the infectious bacteria is present in the throat or nose.
● Inflammation of the nose, throat, and Eustachian tube (the drainage tube between the throat and middle ear)
● Swelling obstructs the narrowest portion of the Eustachian tube.
● Obstruction of the Eustachian tube causes poor ventilation and resultant negative middle ear pressure. This leads to the accumulation of secretions produced in the middle ear.
● The secretions accumulate in the middle ear space creating an ideal environment for growth of bacteria and viruses.
● Viruses and bacteria that colonize the upper respiratory tract enter the middle ear.
● Bacteria or viruses grow in the middle ear secretions resulting in inflammation, fever, pain and bulging of the eardrum which are the symptoms of a middle ear infection.
What are the symptoms of ear infection? The most common symptom of OM is moderate to severe ear pain. This is not universal, especially in younger children and up to 17% of people with OM have no ear pain. Other symptoms include fever, irritability, headache, loss of appetite, vomiting, and diarrhea, but these may be more related to associated respiratory infections than the ear infection itself. The majority of people with OM will have low to moderate grade fever (<104 F) at some point in the illness. Fever may be intermittent and will usually respond to OTC medications such as acetaminophen or ibuprofen. Fever over 104 F is unusual in OM and often is due to another, accompanying infection (e.g. cold or flu).
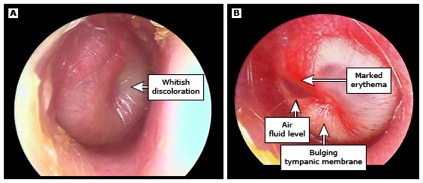
Otitis media is diagnosed by your doctor using an otoscope which is a lighted, funnel-shaped instrument. The most important finding is a red, bulging eardrum (photograph above).
How do we treat ear infections? Bacteria and viruses both cause OM in about equal numbers. In about 2/3 of cases, both can be isolated from middle ear fluid in people with OM. For practical purposes, it’s virtually impossible to differentiate between OM caused by viruses or bacteria. In the past, treatment with antibiotics was almost universal. However, recent evidence indicates that at least half of these illnesses are caused by viruses which cannot be treated with antibiotics. In addition, the majority of people with OM will get better with symptomatic treatment alone (see below). Antibiotics may be associated with significant side effects, allergic reactions and costs. For these reasons, many clinicians to take a ‘wait and see’ approach to antibiotics for OM. With this treatment method, the parent or patient is given a prescription for antibiotics but asked to wait 24-48 hours before starting. If the patient improves, continues to appear well, and the pain and fever are not too severe, then antibiotic therapy is withheld. If the patient fails to improve, antibiotics are initiated. Significant worsening of symptoms should prompt urgent reevaluation by your provider, whether antibiotics have been given or not.
Symptomatic treatment includes OTC medications for fever such as acetaminophen (Tylenol) or ibuprofen (Motrin), fluids by mouth, and rest. Decongestants may enhance middle ear drainage but should not be used in younger children because of side effects (sedation).
Prevention
The occurrence of ear infections can be reduced by avoidance of exposure to cigarette smoke and other irritants, frequent hand-washing to prevent respiratory infection, and treatment of environmental allergies. Daycare centers can help by providing sanitary conditions and asking parents of sick children to keep them at home. Older children should be taught the importance of hand washing and respiratory etiquette (“cover your mouth!”). Providers may refer people with frequent OM to an ear doctor (otolaryngologist) to search for underlying causes such as anatomical abnormalities or immune deficiency.
If you believe you or your child (ages 2 and up) has an ear infection, we encourage you to visit our urgent care clinic, QuickCare of Brevard!